Western NSW Primary Health Network (WNSW PHN) is committed to empowering general practice teams in our region to deliver best patient health outcomes. There are four main stages of Quality Improvement:
- Quality Planning
- Quality Assurance
- Quality Control
- Quality Management
WNSW PHN can provide you with practical advice to assist in implementing Quality Improvement in your practice through our Practice Development Team. Our WNSW PHN has also developed a number of resources to support Quality Improvement activity in our region. These can be found in the 'Related Resources' section on this page.
What is Quality Improvement?
Quality Improvement is a consistent and systematic approach to achieve measurable health outcomes in general practice.
A Quality Improvement approach can be used to review structures, systems and processes to enhance patient care, outcomes and safety.
How do we support Quality Improvement?
Western NSW PHN provides resources and training to support Quality Improvement in general practice. These include:
- Practice Support and Engagement Plans
- Building Block Frameworks
- An Aboriginal Health Business Model
- Accreditation Support
- Digital Health Training and Support
- General Education and Training
Chat with our Practice Development Team to find out more.
Practice Incentive Program (PIP) Quality Improvement
The Practice Incentive Program (PIP) supports general practice activities that encourage continuing improvements, quality care, enhancing capacity and improving access and health outcomes for patients.
The number and type of incentives available within PIP will change from August 1, 2019, when five of the existing incentives will cease and a new incentive, the PIP Quality Improvement (QI) Incentive, will commence.
The QI Incentive aims to recognise and support those practices that commit to improving the care they provide to their patients. Participating practices will be supported to utilise the information they have about their own communities and their knowledge of the particular needs of their own patients to develop innovative strategies to drive improvement.
As well as demonstrating a commitment to quality improvement, practices will share a minimum set of aggregated data with their local Primary Health Network (PHN), such as the number of patients who are diabetic, the percent who smoke, the cardiovascular risk and weight profile.
This information will be collated at the local level by the PHNs to assist in supporting improvement and understanding health needs. There is no requirement for individual patient data, and any measures from an individual practice will not be available to the Department of Health.
With an implementation date of August 1, 2019, the following four Incentives will continue through to July 31, 2019 and then cease:
- Asthma Incentive
- Quality Prescribing Incentive
- Cervical Screening Incentive
- Diabetes Incentive
The seven PIP Incentives that will remain unchanged are:
- eHealth Incentive
- After Hours Incentive
- Rural Loading Incentive
- Teaching Payment
- Indigenous Health Incentive
- Procedural General Practitioner Payment, and
- General Practitioner Aged Care Access Incentive
For ongoing and up-to-date information about the QI PIP from the Commonwealth Department of Health, please click HERE.
PIP Checklists and Activities
| QI PIP Checklists | QI PIP Activities |
- QI Toolkit PIP QI 10 Measures
- QI Toolkit Patient Population
- FAQs
- Pen CS FAQs
- Quality Improvement Guide & Tools
- QI Toolkit Patient Population
- QI Toolkit PIP QI 10 measures
- Quality Improvement Activity Planning Sheet
- COVID-19 Practice Incentive Payment
Bodenheimer's 10 Building Blocks for Primary Care
Bodenheimer's '10 Building Blocks for Primary Care' underpins the success of high-performing primary care.
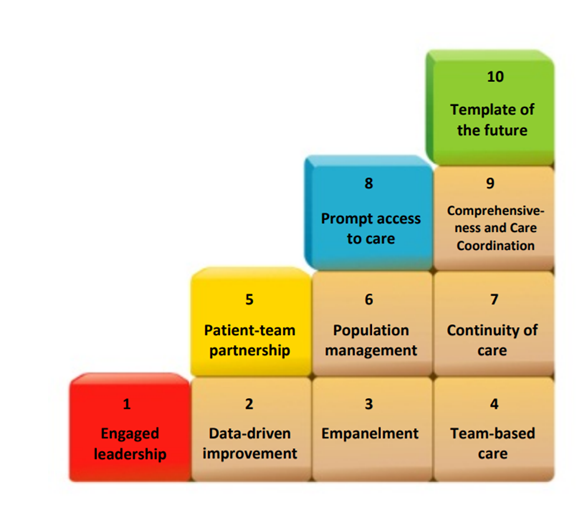
A central component of fulfilling the Bodenheimer's '10 Building Blocks for Primary Care' is to have a person-centred approach.
In a Person-Centred Health System, the person, their families and carers are at the centre of how care and is designed, planned, communicated and delivered. This is because ultimately, it is the values, resources and actions of the person and their carers that are the key determinants of health outcomes.
Every community has differing characteristics and it is ideal for a practice to identify its patient population, particularly if it has a high number coming from priority and diverse populations. These populations might include:
- Aboriginal and Torres Strait Islander
- People living with a disability
- People who identify as part of the LGBTQI community
- Culturally and Linguistically Diverse (CALD)
- Migrants including asylum seekers or those on long-term student visas
- Patients experiencing mental illness
- Homeless people
Ensuring vulnerable patients are identified and treated equitably is important for identifying disease early and for better health outcomes.
Contact Us
WNSW PHN Practice Development Team
practicedevelopmentteam@wnswphn.org.au
Related Resources
Practice Incentives Program Quality Improvement Incentive Factsheet - What practices need to know
Practice Incentives Program Quality Improvement Incentive Factsheet - Consumer
Practice Incentives Program Quality Improvement Incentive - Who do I Ask?
Practice Incentives Program Quality Improvement Measures
Practice Incentives Program Quality Improvement Guidelines
Practice Incentives Program Quality Improvement Measures - Annotated Specifications

